Editor’s note: Dr. William Miller, chief of staff at the Adventist Health Mendocino Coast Hospital, is writing weekly reports concerning the COVID-19 situation on the Mendocino Coast. We are pleased to be running his health column, with details on the medical fight against the pandemic. The views shared in this weekly column are those of the author, Dr. William Miller, and do not necessarily represent those of The Mendocino Voice or of Adventist Health.
As the Delta variant fuels a surge in new cases, we are seeing some people get sick who were previously vaccinated. Does this mean the vaccines are not as effective as they once were?
Before we start, we should draw a few distinctions. First, there is a difference between getting infected and getting ill. Someone can be infected and without symptoms, yet still potentially contagious. An ill person is someone who is infected and has symptoms. We can further divide illness into mild, moderate or severe. With COVID, mild symptoms might include a dry cough, sore throat and headache, while moderate would include getting short of breath when walking across a room or feeling extremely fatigued. Severe symptoms would be having a very low oxygen level requiring treatment with oxygen, these people often require hospitalization. Failure of the lungs to the point of requiring a machine to assist with breathing would be critically ill and those people are in an ICU. Obviously, the next point in the continuum would be those who die of the disease.
Next, we need to consider what is meant when we say a vaccine is “effective”. The goal of a vaccine program is to reduce the infection rate in the population so that the disease does not spread as easily or quickly. This is by both stopping an infection from happening in the first place or if infection occurs anyway then reducing the viral load making the vaccinated person less contagious. Looking at how the disease is spreading in vaccinated versus unvaccinated populations is a way to judge whether a vaccine is “effective” or not. Another purpose of a vaccine is to reduce the severity of illness. Keeping a vaccinated person from progressing to serious illness or death would be considered good effectiveness of a vaccine.
On the other hand, a vaccine does not act as a barrier that will prevent all infections and all illness. No vaccine is 100% effective on all levels. The term “breakthrough” infection is perhaps not helpful as it seems to imply that somehow the virus “broke through” such a barrier. There will always be a small percentage of fully vaccinated people who get sick, are hospitalized, and even die from COVID-19. To judge the effectiveness of the vaccine we must compare the rates of serious illness and death in vaccinated versus unvaccinated people.
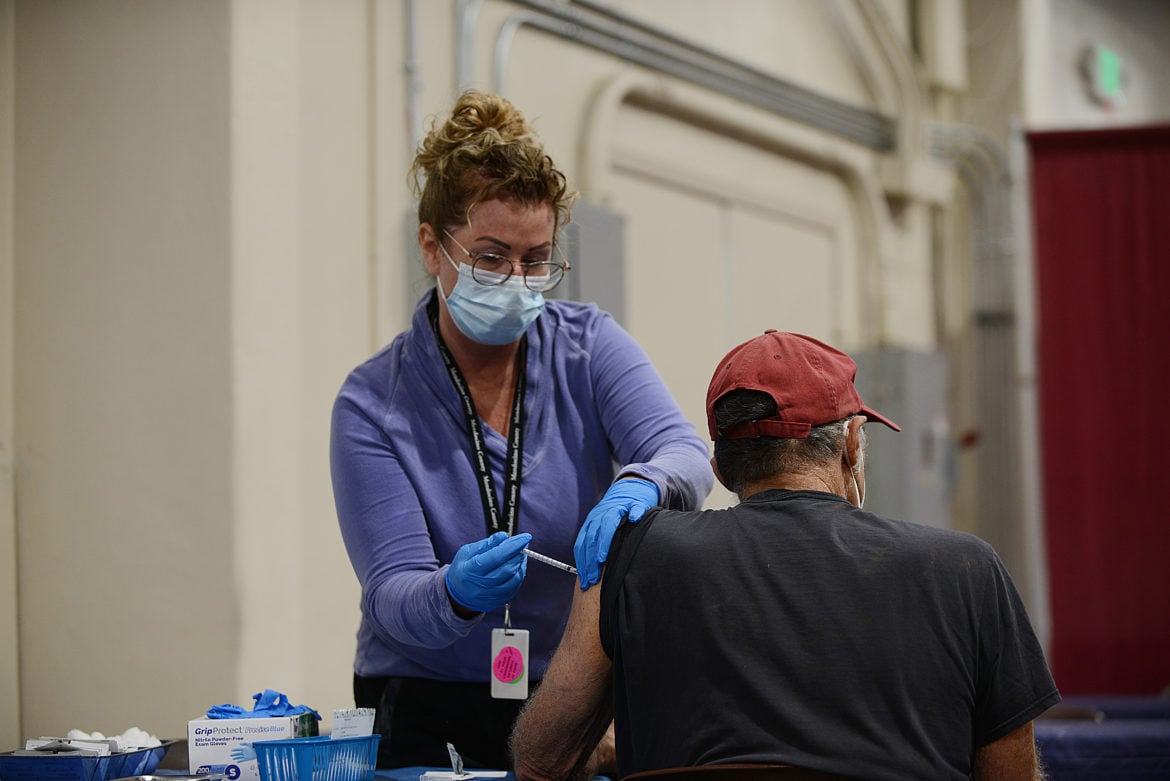
The vast majority of new cases across the US and locally are in unvaccinated people. According to the CDC, 99.6% of all new cases are in unvaccinated persons. The California Department of Public Health website indicates that for the week of August 9 – August 15, the average case rate among unvaccinated Californians was 51 per 100,000 per day while the average case rate among vaccinated Californians was significantly lower at 7.6 per 100,000 per day. They went on to state that there is a 500% higher risk of infection for unvaccinated persons right now compared with vaccinated persons. This is strong evidence that the vaccines do work in protecting against new infections even against Delta which now makes up well over 85% of all infections.
So, if this is true, then why are we still seeing cases? The reason is that if the vaccine protects against 92% of infections, that still means that 8% of people who are vaccinated can become infected if exposed. For example, if there is a large group of vaccinated people getting together with a large number of unvaccinated and potentially infected people, then you will see many vaccinated people coming down with COVID. This is the explanation of what happened in Barnstable County, Massachusetts, in July. Mask mandates and restrictions on public gatherings had been relaxed. During that month, there were several very large entertainment events bringing in thousands of participants and tourists. Despite having a large percentage of vaccinated people (69%) the community experienced an outbreak that included 346 vaccinated people. It is important to note, however, that only 4 of those vaccinated people required hospitalization and none died.
Perhaps most importantly, the vaccines remain effective in protecting against serious illness, hospitalization and death. A study of 7,280 vaccinated COVID patients was reported in the Morbidity and Mortality Weekly Report (MMWR) on August 13th stating “Among adults aged 65-75, effectiveness of full vaccination for preventing hospitalization was 96% for Pfizer-BioNTech, 96% for Moderna and 84% for Janssen COVID-19 vaccines; among adults aged >75 years, effectiveness of full vaccination for preventing hospitalization was 91% for Pfizer-BioNTech, 96% for Moderna and 85% for Janssen…” While this study is very helpful, there are two limitations. First, it looked at cases between February and April, 2021, which was prior to Delta becoming the predominant variant. Second, most of the people in the study had been recently vaccinated. Other studies have suggested that the rate of protecting against hospitalization with Delta is around 88% for Pfizer and Moderna as reported in the New England Journal of Medicine on July 21st.
There is evidence that the effectiveness of these vaccines does wane over time. A very robust study involving over 740,000 people in the United Kingdom was just published in the journal Nature on August 19th. Half of the study took place early in 2021 when the Alpha variant predominated and the other half was in the last three months when Delta predominated. Participants had all received either both doses of Pfizer or the single dose of AstraZeneca. It looked at the effectiveness of protecting a fully vaccinated person against infection by assessing viral load following a known exposure. The study found that the Pfizer vaccine “was 92% effective at keeping people from developing a high viral load… 14 days after the second dose. But the vaccine’s effectiveness fell to 90%, 85% and 78% after 30, 60 and 90 days, respectively.” Keep in mind that even at 78%, this is still considered good. This study only looked at viral load as an indicator that the person might be infectious but it did not look at whether or not the subjects developed symptoms or got hospitalized. However, it does support the notion that a booster shot at some point may be beneficial.
Next week we will look at the use of monoclonal antibody treatments to prevent progression to severe COVID, in particular the Regen-COV preparation by Regeneron. You can access previous Miller Reports by visiting www.WMillerMD.com.
The views shared in this weekly column are those of the author, Dr. William Miller, and do not necessarily represent those of the publisher or of Adventist Health.




“They went on to state that there is a 500% higher risk of infection for unvaccinated persons right now compared with vaccinated persons. This is strong evidence that the vaccines do work in protecting against new infections even against Delta which now makes up well over 85% of all infections.”
So the CDC makes a crazy statement and that is now considered “evidence”!?
You know this sure smells fishy and the CDC would NEVER paint the unvaxxed in a negative light… or skew numbers to make it look like unvaxxed (unclean) individuals are the problem. Why didn’t the good Dr cite the case with the fully vaxxed cruise ship that was peppered with cases left and right!? Geez how on earth could that have happened!? Israel which is mostly vaxxed having many “breakthrough” cases.. oh noooo don’t mention that, it’ll destroy the narrative.
Imagine if these Dr.s treated people early with therapeutics, and they recovered and therefore received mucosal immunity! Like my brother, cousin, niece friends all have now, then you wouldn’t need some BS experimental mystery drug injection that fades with efficiency! hmm…
This is certainly the spin the vaccine makers are putting out along with the propagandists in the corporate media. This overlooks the reality that the task Operation Warpspeed gave them was to produce a safe and effective vaccine that prevented patients from becoming infected with SARS-CoV-2 or transmitting it. At the end of 2020, when it became apparent that none of the vaccines marketed in the Western World significantly reduced infection or transmission, instead of scrapping the project and attempting to produce a vaccine that did reduce infection and transmission, they (and their friends at the FDA and CDC) opted to move the goal posts and foist a vaccine on the public that appeared to reduce the severity of SARS-CoV-2 infection. I say appeared to reduce severity, only because (as the British Medical Journal has pointed out) they refused to release their data for independent review. With the appearance of the Delta variant (which many virologists with experience with coronaviruses predicted), it’s now questionable if the Pfizer vaccine at least (the main vaccine used in Israel) significantly reduces the risk of hospitalization and death.
In dealing with the question of reducing hospitalization and death, there are several safe and effective treatment options that are peer reviewed. These include Ivermectin (which has been shown to reduce death rates by 85% in 49 peer reviewed studies), hydroxychloquine and monoclonal antibodies. Sadly this information is being suppressed by the Western media, though Ivermectin is being widely used in third world countries.
Courtesy of Stew Bramhill.
Dr. William Miller,
How much 2020 CARES Act money/funding do your Hospital, Administration and Board receive for each Covid patient admitted, administered Covid test, ICU ventilator used for diagnosed Covid patient, Medicare patients diagnosed with Covid?
Covid-19 HUSH MONEY: $2.2 Trillion CARES Act coercion
Hospitals were being paid to diagnose Covid.
Most people don’t know that. All you have to do is type in ‘CARES Act 2020 reimbursement’ for your hospital to discover this information, but I thought I would ask you for an honest assessment first.
Yeah keep on digging those heels in and standing firm with your alternative news brethren. Surely the facts and figures shared by the hospital chair are all merely spin, generated by the big corporate government media machine whose only real goal is to make money, which makes them purely corrupt and therefore everything these organizations and their puppets say and do is suspect. (Because under our Lord’s beloved capitalism, the pursuit of profit is the only functional goal.) Meanwhile, it’s a fantastic idea to ingest malaria drugs and now livestock parasite treatments while avoiding the dreaded jab at all costs. Don’t trust the prescribed lies of Big Pharma! Take different drugs created also by pharma companies but for completely different reasons instead. That’s your right as an American, and when the Grand Old Party returns to power, the DemonRats – who are fully representative of any and all ideas you might identify as “radical left” – will lose everything and be defeated forever. Then God’s favorite President will come back and American Values (whatever we think those are) will reign supreme! So to all the intelligent Anti-Vaxxers right here in Mendocino county, I say Salutations and Amen